Five Smart Moves to Strengthen and Optimize Your Pharmacy Benefit Plan
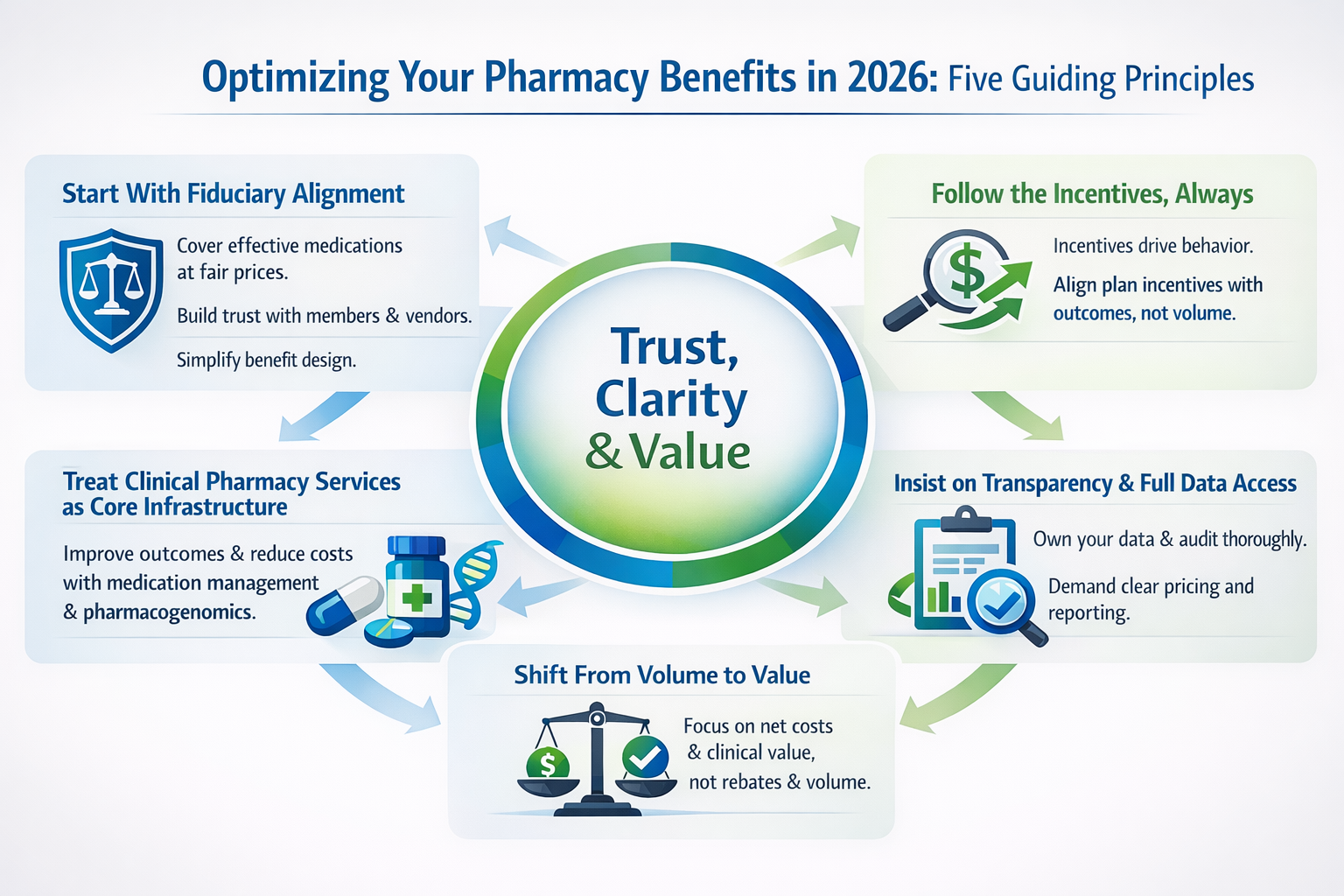
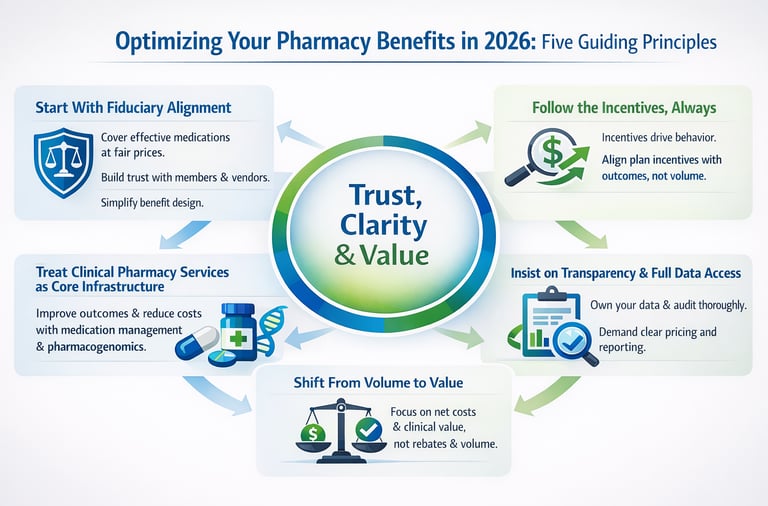
In 2026, employers must refocus on five priorities: uphold fiduciary responsibility, fix misaligned incentives, invest in independent clinical pharmacy services, demand true transparency, and move from volume-driven to value-based purchasing to better control costs and improve outcomes.
PHARMACY
By Michael Lee, PharmD
1/29/20264 min read
As I reflected on the first month of 2026, one thing stood out: many of the pressures employers faced in 2025 haven’t eased; in fact, they are intensifying. Rising costs, misaligned incentives, and unclear decision-making continue to shape the employer-sponsored healthcare landscape. These challenges are especially visible in pharmacy benefits, where they often appear more quickly and have a greater financial impact.
With that in mind, I took a step back to identify several key themes from last year and explore what they mean specifically for pharmacy benefits. Viewed through this lens, these insights provide a practical guide for employers to refine their strategy and make more deliberate choices.
Below, I’ve distilled these themes into five guiding principles to help optimize your pharmacy benefits plan as you head into 2026.
Start With Fiduciary Alignment
If you sponsor a health plan, you are a fiduciary. That responsibility is not abstract. It means you are obligated to ensure the plan pays reasonable prices for services that meaningfully improve health.
In pharmacy, that translates to a simple but often violated principle: cover medications that work, at prices that make sense, and be disciplined about limiting spend on drugs that add marginal clinical value at an outsized cost.
Trust sits at the center of this obligation. Trust between you and your members. Trust between you and your vendors, whether they are PBMs, consultants, or other service providers. Trust between members and their clinicians. Unfortunately, pharmacy benefits is an environment where trust has been eroded by opaque pricing, conflicted incentives, and unnecessary complexity.
You cannot fix the entire system, but you can decide who you do business with. You can demand straightforward explanations, clean contracts, and behavior that aligns with your interests and your members’ health. Vendors that cannot or will not operate that way should not be long term partners.
Simplicity matters here more than most employers realize. If you cannot clearly explain how your pharmacy benefit works, how drugs are priced, and how money flows through the system, you are exposed. Complexity is often marketed as sophistication, but in pharmacy benefits it is more commonly used to obscure true costs. Simpler designs are easier to audit, easier to trust, and far more likely to support reasonable pricing for effective therapy.
Follow the Incentives, Always
Healthcare outcomes almost always follow incentives, and pharmacy benefits is no exception.
The PBM model is a textbook example. When revenue grows with prescription volume and with higher list prices through rebates, it should not surprise anyone that formularies drift toward higher cost drugs. The system is doing exactly what it was built to do.
PBMs are not the only place where incentives are misaligned. Many brokers and consultants receive compensation from PBMs, creating a pay to play dynamic in procurement decisions. When your advisor is paid by the vendor they are recommending, you should at least pause and ask whether your interests are truly the priority.
Cost sharing is another area where intentions and outcomes diverge. Higher out of pocket costs are often justified as a way to discourage waste. In practice, they frequently lead to cost related nonadherence, where members skip doses, delay refills, or abandon therapy altogether. The downstream consequences show up later as worsening chronic disease, avoidable complications, and higher total costs.
A useful rule of thumb applies here: incentives predict behavior. If you want different outcomes, you must redesign the incentives that drive drug selection, utilization, and adherence across your plan.
Treat Clinical Pharmacy Services as Core Infrastructure
Poor medication use is not a niche problem. Incorrect dosing, inappropriate therapy, adverse effects, and nonadherence collectively account for a massive share of healthcare spend.
That reality should fundamentally change how employers think about clinical pharmacy services. These services are not add ons. They are infrastructure.
Comprehensive medication management, when done well, ensures that each medication a member takes is appropriate, effective, safe, and actually being used as intended. The evidence is clear that these programs reduce hospitalizations and emergency department visits and lower total cost of care.
Pharmacogenomics testing adds another layer by helping match patients to medications that are more likely to work for them based on their genetic profile. This is not futuristic medicine. It is increasingly practical, and when deployed thoughtfully, it improves outcomes while avoiding costly trial and error prescribing.
One important caveat: independence matters. Vendors providing these services should not benefit financially from recommending one drug over another. If incentives are layered on top of clinical recommendations, the value of the service erodes quickly.
Insist on Transparency and Full Data Access
Opacity in pharmacy benefits is not just frustrating, it is risky.
Without clear visibility into pricing methodologies, formulary decision making, and vendor revenue streams, you cannot effectively manage spend or meet your fiduciary obligations. Marketing labels like “transparent PBM” are not substitutes for enforceable contract language and audit rights.
Transparency also means owning your data. Not summary reports, not curated dashboards, but full prescription level claims data. If you do not have that access, there is almost certainly money leaking out of your plan.
Under the Consolidated Appropriations Act, employers have the right to their data and the responsibility to use it. Independent analysis is not optional if you want to understand true net costs, utilization patterns, and opportunities for improvement.
Shift From Volume to Value
The current purchasing framework rewards volume. In pharmacy, that shows up most clearly through rebates and rebate driven formularies.
When formulary placement is dictated by rebate size rather than clinical value and net cost, the system predictably favors higher priced drugs, even when lower cost alternatives perform just as well. This structure makes value based purchasing nearly impossible.
Employers can push back. Ask how value is defined in formulary decisions. Demand lowest net cost rather than highest rebate. Adopt biosimilars first strategies and be intentional about how new high cost therapies are evaluated and introduced.
Volume based purchasing may boost PBM revenue, but it does so at the expense of plan sponsors and members. Value based purchasing aligns dollars with outcomes, which is where they belong.
Closing Thoughts
Optimizing pharmacy benefits can feel overwhelming, especially given how entrenched many of these problems are. But progress does not require perfection. It requires clarity, discipline, and a willingness to challenge long standing assumptions.
As you look toward 2026, these five principles provide a practical starting point. Align with your fiduciary duty. Question incentives. Invest in clinical pharmacy services. Demand transparency. And shift your purchasing strategy from volume to value.
Pharmacy benefits can work better. But only if employers insist that they do.